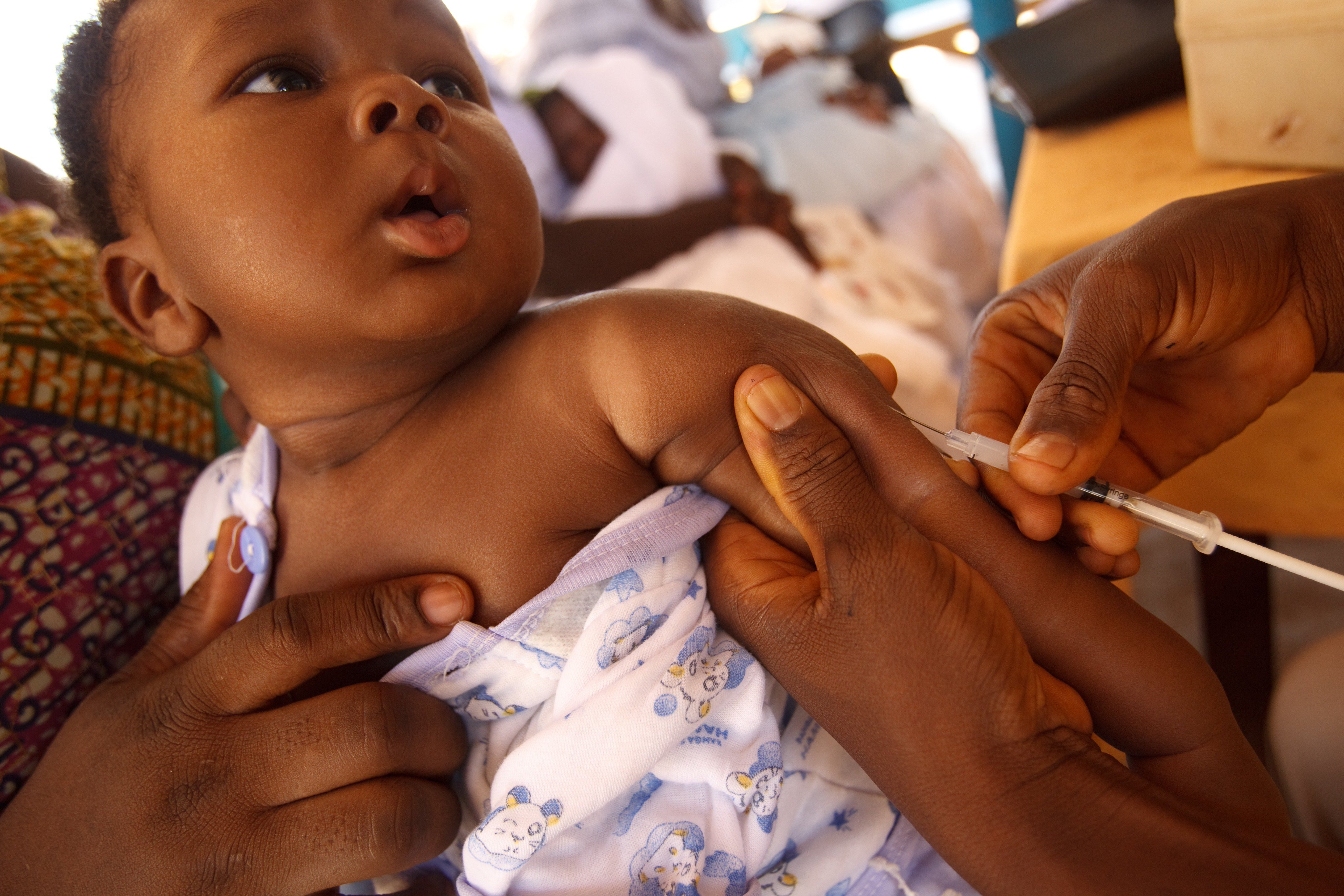
The World Health Organization (WHO) has suggested widespread use of RTS,S/AS01 (RTS,S) malaria vaccine among children in sub-Saharan Africa and other regions with moderate to high P. falciparum malaria transmission.
Results from an ongoing pilot program in Kenya, Ghana and Malawi informed the suggestion.
The program has reached over 800,000 children since its start in 2019.
WHO Director-General Dr Tedros Adhanom Ghebreyesus said the vaccine is a breakthrough for science and it could save young lives annually.
“This is a historic moment. The long-awaited malaria vaccine for children is a breakthrough for science, child health and malaria control. Using this vaccine on top of existing tools to prevent malaria could save tens of thousands of young lives each year,” Ghebreyesus said.
Read More
More than 260,000 African children under the age of five die annually of malaria, as it remains a primary cause of childhood illness and mortality in sub-Saharan Africa.
WHO and its partners have reported stagnation in the progress against malaria in recent years.
WHO Regional Director for Africa Dr Matshidiso Moeti said malaria has stalked sub-Saharan Africa for centuries, causing immense suffering and hope for an effective vaccine is rejuvenated.
"For centuries, malaria has stalked sub-Saharan Africa, causing immense personal suffering. We have long hoped for an effective malaria vaccine and now for the first time ever, we have such a vaccine recommended for widespread use. Today’s recommendation offers a glimmer of hope for the continent which shoulders the heaviest burden of the disease and we expect many more African children to be protected from malaria and grow into healthy adults,” Moeti said.
WHO recommends that in the context of comprehensive malaria control, the RTS,S/AS01 malaria vaccine be used for the prevention of P. falciparum malaria in children living in regions with moderate to high transmission as defined by WHO.
RTS,S/AS01 malaria vaccine should be provided in a schedule of 4 doses in children from 5 months of age for the reduction of malaria disease and burden.
The following is a summary of key findings of the malaria vaccine pilots based on data and insights generated from two years of vaccination in child health clinics in the three pilot countries, implemented under the leadership of the Ministries of Health of Kenya, Ghana and Malawi.
Feasible to deliver: Vaccine introduction is feasible, improves health and saves lives, with good and equitable coverage of RTS,S seen through routine immunization systems. This occurred even in the context of the COVID-19 pandemic.
Reaching the unreached: RTS,S increases equity in access to malaria prevention.
Data from the pilot programme showed that more than two-thirds of children in the 3 countries who are not sleeping under a bednet are benefitting from the RTS,S vaccine.
Layering the tools results in over 90% of children benefitting from at least one preventive intervention (insecticide-treated bednets or the malaria vaccine).
Strong safety profile: To date, more than 2.3 million doses of the vaccine have been administered in 3 African countries – the vaccine has a favourable safety profile.
No negative impact on the uptake of bednets, other childhood vaccinations, or health-seeking behaviour for febrile illness. In areas where the vaccine has been introduced, there has been no decrease in the use of insecticide-treated nets, uptake of other childhood vaccinations or health-seeking behaviour for febrile illness.
High impact in real-life childhood vaccination settings: Significant reduction (30%) in deadly severe malaria, even when introduced in areas where insecticide-treated nets are widely used and there is good access to diagnosis and treatment.
Highly cost-effective: Modelling estimates that the vaccine is cost-effective in areas of moderate to high malaria transmission.